
The COVID-19 pandemic changed the healthcare landscape dramatically and permanently. Early in the pandemic, lockdowns and state-led rulings caused a pause in many types of elective care, and best practices led to patients only coming in when it was absolutely necessary. Even beyond the initial stages of the pandemic, some patients avoided care to prevent the risk of COVID-19 infections.
This delay and avoidance of care introduced many problems for the healthcare world. Elective care drives much of practitioner revenue, which in turn impacted care providers’ businesses. Patients, meanwhile, were going without care — serious conditions were going undiagnosed and untreated, and many with chronic conditions found them worsening without guidance. With traditional care channels no longer an option for many, patients turned to non-traditional channels, making use of technology such as remote care visits, remote patient diagnostics, remote patient monitoring platforms, and other virtual care modalities.
Regulators also took notice of the need for remote care, making massive changes to the reimbursement and regulatory landscape. Many care providers were reimbursed for remote visits at a similar scale to in-person, and the number of conditions people could seek treatment for dramatically widened. Hospitals and care providers quickly pivoted their strategies in response, rapidly launching their own platforms using whatever technology they had available, and soon, many patients could simply schedule a visit with their regular physician. The use of connected health devices also skyrocketed, as providers and payers realized that they needed biometric data to augment remote visits and make appropriate care decisions.
The threat of COVID-19, loss of elective care revenue, and rapid pivot to telehealth led to a sea change in how technology is perceived and used by care providers and health systems. It is no longer a threat — instead, it has become a valuable tool they can leverage. Companies are now more open and eager to figure out more effective ways of building new best practices around their use of technology.
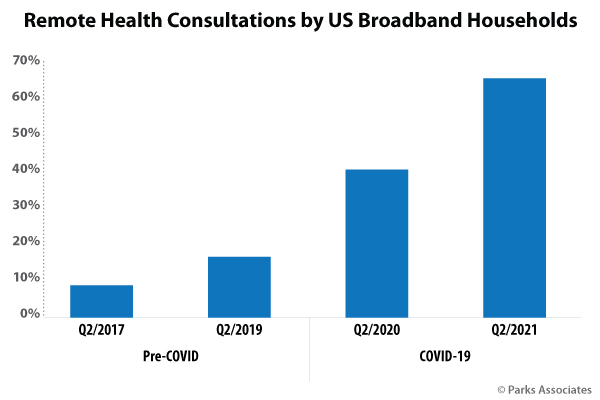
Parks Associates has studied the telehealth and remote care market for over five years, fielding demographically representative surveys to 5,000 heads of U.S. broadband households. Since 2017, there has been an exponential increase in the adoption of remote health consultations by patients, which dramatically accelerated with the advent of the COVID-19 pandemic. As of today, almost two-thirds of U.S. broadband households have reported performing at least one remote health consultation in the past 12 months alone. This new reality isn’t something that healthcare players can afford to ignore, or that they can hope will go away; it’s here to stay.
And likewise, increased adoption of connected health devices and programs has continued. As of Q2 2021, over half of U.S. broadband households now own and use an Internet-connected health or fitness device that captures biometric data. These devices include a mix of products purchased at retail or received from employers, payers, and care providers.
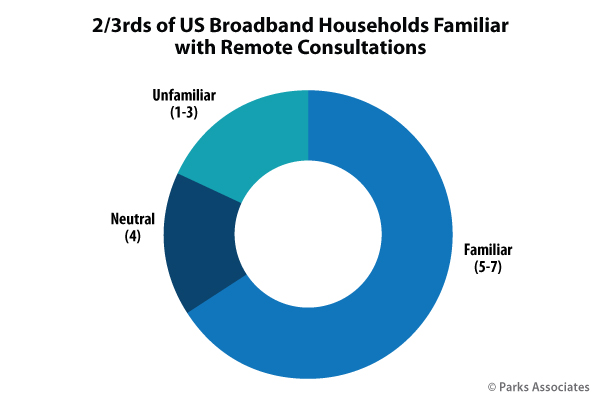
When it comes to actual participation in medical programs that use data gathered from devices at home — that is, remote patient diagnostics, remote patient monitoring, etc. — 40 percent of U.S. broadband households report participating in such a program at least once during their lifetime. Additionally, when asked how they felt about sharing device data with clinicians, over 60 percent of survey respondents found at least one of our tested models to be “appealing” as rated on a seven-point scale.
Many consumers make regular use of health devices, and many have been touched by actual medical devices at least once in their lives. Many are also open to further engagement with these types of programs. As there are a variety of connected-device types and the data they collect, there are many different types of use cases — ranging from programs such as Livongo’s, designed to improve diabetes outcomes, to programs designed to monitor congestive heart failure patients post-discharge, or to remote diagnostic solutions such as TytoCare’s, that allow physicians to read a patient’s biometric data during a consultation. Use cases run the gamut from the more established use case of remote-patient monitoring for chronic-condition monitoring or monitoring after discharge from the hospital to diagnostic support for telehealth consultations.
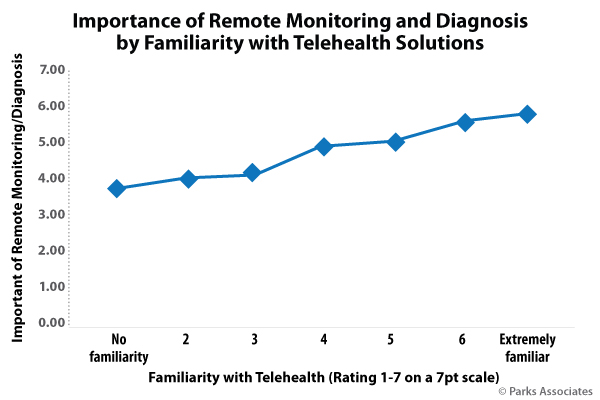
Growing familiarity with telehealth has helped drive the expanded connected health device market. Parks Associates’ research shows that there is a strong linear correlation between familiarity and wanting the benefits that connected health devices bring in terms of remote diagnostics and remote monitoring.
Looking at the overall landscape for health tech, there are, of course, a great number of additional applications and use cases such as software as a medical device, decision support and triage tools, patient assessment tools, risk identification and patient population stratification, automated care platforms, clinician workflow management, and others. The use of these tools is likewise increasing, and investment in the virtual and connected health space is at an all-time high, as regulators further move to make permanent certain expanded reimbursement and further loosen regulatory requirements (see National Law Review: https://www.natlawreview.com/article/cms-addresses-virtual-care-expansion-cy-2022-medicare-physician-fee-schedule).
For more information on how IoT sensor data and connected health and related devices are transforming healthcare functions into data-driven services, please visit the Parks Associates website at www.parksassociates.com or register for Parks Associates’ 8th Annual Connected Health Summit by visiting www.connectedhealthsummit.com














